[Fournier2008] presents evidence that coadministration of bio-identical estrogen and progesterone
does not increase the risk of invasive breast cancer, whereas administration of unopposed estrogen or non-bioidentical
progestins (e.g. Provera™ = medroxyprogesterone acetate = MPA) does significantly increase the risk of breast cancer, as previously reported
by the Women's Health Initiative (WHI) study [Beck2012].
Numerous other studies support the relative safety of bio-identical hormones given in
physiological doses, compared with patented non-bio-identical pharmaceutical "frankenhormones": [Holtorf2009], [Moskowitz2006],
[Birrell2007].
In addition, multiple studies show that use of oral contraceptives (containing non-bio-identical hormones) are linked with higher
risk of breast cancer [Collaborative_Group1996]; in particular, the progestin
levonorgestrel (Plan B One-Step) appears to be especially problematic
[Hunter2010].
This issue has also been discussed in the popular press: [Somers2006], [Somers2009], [Somers2012],
[Lee2002].
Based on a study of three castrated patients with advanced carcinoma of the prostate gland,
[Huggins1941] made the sweeping generalization that "giving testosterone to a man
with prostate cancer is like adding oil to a fire." Subsequent studies of rats by [Noble1977] and humans
[Fowler1981] reinforced the notion that testosterone promotes prostate cancer.
Although Huggins was awarded a Nobel Prize for his work, and his theory has long been taught in medical schools, it has recently
been shown to be almost diametrically false. In particular, Huggins' model fails to account for the role of estrogen, dihydrotestosterone (DHT),
or hormone receptors in the promotion of prostate cancer.
More recently, [Morgentaler2008] has pointed out that prostate cancer is more prevalent
in men with low testosterone, and that in most cases, supplementing with testosterone is actually safe and beneficial [Morgentaler2011],
[Szmulewitz2009], [Morris2009], [Isaacs2012].
As will be discussed below, testosterone itself is protective; however, its metabolites
estradiol (E2) and dihydrotestosterone (DHT) are the hormones actually responsible for initiating breast and prostate cancer.
[Friedman2013] makes the case (see below) that without both E2 and DHT, initiation of breast or prostate cancer is not possible,
and that lowering local E2 and DHT levels reduces the risk of these cancers.
It is important to distinguish between systemic levels of E2 and testosterone arising from bio-identical hormone replacement therapy
(and measured in blood, urine, or saliva), versus the cancer-forming
high local levels of E2 and DHT arising from excessive conversion of testosterone to E2 or DHT inside the breast or prostate tissue.
[Friedman2013] further points out that in addition to high local levels of E2 and DHT, these hormones must interact with hormone receptors
in the breast and prostate named Estrogen-Receptor-alpha (ER-alpha) and Membrane-bound
Androgen Receptor (mAR), respectively, in order to induce cancer, as described further below.
Apoptosis (also known as "programmed cell death") is a process that protects the body from
defective or old cells, and is triggered by the immune system when a cell appears to be problematic.
Cellular apoptosis is modulated by the balance between competing pairs of hormone receptors,
which control expression of the tumorigenic protein
BCL2
versus the anti-tumor protein TP53,
as discussed below [Friedman2007].
BCL2 is a key protein involved in the control of apoptosis, which is in turn regulated by opposing
pairs of cellular hormone receptors [Kandouz1996]:
- Estrogen-receptor-alpha (ER-alpha) versus estrogen-receptor-beta (ER-beta)
- Progesterone-receptor-alpha (PR-alpha) versus progesterone-receptor-beta (PR-beta)
- Membrane androgen receptor (mAR) versus intracellular androgen receptor (iAR)
In each of these pairs of hormone receptors, the first receptor increases expression of the
tumorigenic protein BCL2, which acts to protect the cell against normal apoptosis, thus promoting
cancer.
In addition, mAR decreases the production of the protective protein AS3, while iAR increases the
production of the protective protein AS3 [Friedman2013, pg 60].
Estrogen
It is useful to compare the relative affinities of the three main types of estrogen found in humans: estrone (E1), estradiol (E2),
and estriol (E3) [Friedman2013]:
Relative binding strengths of estrogen receptors for different estrogens
| Receptor | Estrone | Estradiol | Estriol
|
|---|
| ER-alpha | 0.1 | 1.0 | 0.11
|
| ER-beta | 0.02 | 1.0 | 0.35
|
As we see above [Zhu2006], [Friedman2007]:
- E1 has an affinity for ER-alpha that is 5 times greater than for ER-beta, and thus promotes tumor development.
- E2 has an equal affinity for ER-alpha and ER-beta, and promotes tumor development when ER-alpha predominates.
- E3 has an affinity for ER-beta that is 3.5 times greater than for ER-alpha, and therefore is protective.
- However, E3 binds to ER-beta only 35% as strongly as E2 does, so maximum protection provided by E3 requires that
E2 levels be low.
ER-beta is also beneficial by reducing inflammation that is often seen accompanying both benign prostate hypertrophy (BPH) and prostate cancer
[Risbridger2007],
which Dr. Weyrich suggests that inflammation is not a cause of prostate cancer, but rather an effect (marker) of low ER-beta activity.
It is not clear [to Dr. Weyrich] whether ER-alpha itself promotes production of the antiapoptotic protein BCL2, or whether either
the homodimer formed by two ER-alpha receptors, or the heterodimer formed by one ER-alpha combining with one ER-beta is the culprit.
In any case, high levels of ER-alpha promote formation of both the homodimer and the heterodimer, and high levels of estradiol promote
simultaneous activation of both receptor regions in either the homodimer or the heterodimer [Friedman2013, pg 48].
[Ricke2008] has shown that ER-alpha [Dr. Weyrich: or its homodimer or heterodimer] is necessary for the formation of prostate cancer,
which Dr. Weyrich considers to draw attention to ER-alpha, with the discussion of its homodimers and heterodimers being an interesting detail.
[Lofgren2006] has shown that in normal breast tissue, the activity of ER-alpha and ER-beta are equal, and on balance does not promote
breast cancer.
However, once cancer has been initiated, natural selection tends to increase the density of ER-alpha
relative to ER-beta, since the more ER-alpha and the less ER-beta a cell has, the more bc-2 (BCL2?)
is produced, and the greater protection the cell has against apoptosis
[Friedman2013, pg 51].
There is also a third kind of estrogen receptor, which is bound to the cell membrane (mER). Like ER-alpha,
it promotes production of the antiapoptotic protein BCL2 (at least in the case of breast cancer [Friedman2007];
it has not been studied in relation to prostate cancer, but Dr. Weyrich expects a similar action in the case of prostate cancer.
Based on the above, [Friedman2013] presents compelling evidence regarding the cause of prostate and breast cancer,
and a clear model, The Hormone Receptor Model, for both preventing and treating both these cancers, which are primarily driven by
hormonal imbalances, especially excess local tissue (not systemic serum) levels of estradiol on pro-carcinogenic estrogen-receptor-alpha (ER-alpha)
[Bonkhoff2008]. [Friedman2013, pg 81] lists five factors are necessary to initiate prostate cancer:
testosterone, dihydrotestosterone, estradiol, intracellular androgen receptor, and estrogen-receptor-alpha.
Dr. Weyrich notes, however, that evidence presented by Friedman exonerates testosterone as a direct causative agent -
if the conversion of testosterone to dihydrotestosterone and estradiol is blocked (e.g. by 5-alpha-reductase and aromatase inhibitors, respectively)
then testosterone is NOT sufficient to initiate prostate cancer - see below.
Note that the enzyme aromatase converts testosterone into estradiol, and 5-alpha-reductase converts testosterone to DHT,
so inappropriate testosterone supplementation
can indirectly promote both prostate and breast cancer (by increasing telomere length and thus preventing apoptosis of tumorigenic cells),
if aromatase activity is not controlled [Friedman2007].
Support for this theory comes from a study in mice that shows that in the absence of ER-alpha, testosterone cannot induce cancer
[Ricke2008].
Progesterone
PR-beta is beneficial, since it up-regulates
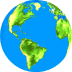 TP53,
which stops cancer growth [Lee2002] by at least three different mechanisms: promoting apoptosis of defective cells, assisting in DNA repair,
and inhibiting angiogenesis [Friedman2013, pg 88].
TP53,
which stops cancer growth [Lee2002] by at least three different mechanisms: promoting apoptosis of defective cells, assisting in DNA repair,
and inhibiting angiogenesis [Friedman2013, pg 88].
There are also two
 membrane progesterone receptors:
mPR-5-alpha and mPR-4.
mPR-5-alpha binds to 5-alpha-pregnanes ("bad progesterone")
that is formed by the action of 5-alpha-reductase, and promotes cancer growth.
mPR-4 binds 4-pregnenes ("good progesterone") and inhibits cancer growth in breast tissue
[Wiebe2000].
These receptors have not been studied in relation to prostate cancer,
but Dr. Weyrich expects a similar action in the case of prostate cancer.
membrane progesterone receptors:
mPR-5-alpha and mPR-4.
mPR-5-alpha binds to 5-alpha-pregnanes ("bad progesterone")
that is formed by the action of 5-alpha-reductase, and promotes cancer growth.
mPR-4 binds 4-pregnenes ("good progesterone") and inhibits cancer growth in breast tissue
[Wiebe2000].
These receptors have not been studied in relation to prostate cancer,
but Dr. Weyrich expects a similar action in the case of prostate cancer.
The BRCA-1 and BRCA-2 genetic mutations disable the protective function of the PR-beta, leaving the tumorigenic PR-alpha unopposed reign.
In persons possessing the BRCA-1 or BRCA-2 genetic mutations, progesterone supplementation is likely to promote prostate and/or breast cancer
[Friedman2007].
Androgens
Cellular apoptosis is also modulated by the balance between intracellular androgen receptor (iAR) and membrane androgen receptor (mAR).
iAR down-regulates production of the tumorigenic BCL2, but mAR up-regulates production of BCL2.
The enzyme 5-alpha-reductase type II (5AR2) converts testosterone to dihydrotestosterone (DHT).
DHT has been shown to bind 5 times more strongly to mAR than testosterone, thereby having the net effect of being tumorigenic, whereas
testosterone favors the protective iAR.
Note however, that the androgen receptors have multiple functions, some of which are protective and some tumorigenic
[Friedman2007, pg 55].
The synthetic progestin Provera™ blocks iAR and thereby disrupts the protective effect of testosterone binding at that site [Birrell2007];
Other researchers have also noted that Provera™ disrupts estrogen receptors as well. Dr. Weyrich notes that, based on Le Chatelier's Law of Mass Action,
supplementing with extra testosterone when Provera is administered can competitively overcome the blockage at iAR by Provera™.
Vitamin D
Vitamin D also has an important role in modulating apoptosis.
The active form of vitamin D is 1,25-dihydroxy-vitamin-D3 (calcitriol), which is formed in the kidneys.
Calcitriol binds to the vitamin D receptor (VDR) and increases cell death in both breast cancer [Narvaez2001]
and prostate cancer [Guzey2002].
Low Vitamin D status therefore is expected to increase the risk of both breast and prostate cancer.

 TP53
TP53